Inactive EGFR found to be assisting in cancer cell survival

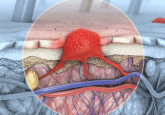
In healthy cells, the EGFR functions for the benefit of the cell. However, the gene controlling EGFR can be reprogrammed in cancer cells, such as in ovarian and skin cancers, and rare aggressive cancers like glioblastoma. This results in overproduction of EGFR, which in turn allows growth to go unchecked and cancer cells to spread.
Xiaojun Tan, a graduate student in Richard A Anderson’s lab at the University of Wisconsin-Madison was investigating the different locations of EGFR in cells, when he came across an unexpected finding. He observed how cancers are able to evade the treatments that are so specifically targeted at shutting down the cellular receiving dock, EGFR.
Tan observed that EGFR-targeting drugs were doing exactly what they were designed to do – inactivating EGFR – however, the cancer cells were using the inactive EGFR as an alternative mechanism for cancer survival. The findings could have huge implications for human health, and also economically for drug developers.
“Hundreds of thousands of patients every year have tumors addicted to EGFR,” commented Anderson. “It has implications for millions of cancer patients worldwide.”
The researchers demonstrated that cancer cells were using the inactive EGFR in autophagy, which often occurs when resources are low or the cell is under stress. During autophagy, cells consume their own nonessential components to conserve energy for survival. Cancer cells also harness this process to aid survival in stressful conditions, for example when tightly packed in a tumor.
When cancer cells have excess EGFR, another protein termed LAPTM4B is found at high levels, which helps to move the inactive EGFR to the location where autophagy starts. The inactive EGFR then plays a role in initiating the cascade of cellular interactions that trigger autophagy, aiding cancer cell survival.
Anderson further commented that it is the first time LAPTM4B has been implicated in initiating autophagy, although the study also found that it is not required for EGFR to trigger the cascade if inactive EGFR finds another means of reaching the autophagy machinery.
The findings suggest that an extra drug should be combined with original EGFR inhibitors to block autophagy and thus potentially block this survival mechanism. “We predict it could be an incredibly effective way of treating cancers,” concluded Anderson, who notes both types of drugs already exist and have US FDA approval. “It could have potentially a very rapid impact on cancer treatment.”
Source: Tan X, Thapa N, Sun Y, Anderson RA. A kinase-independent role for EGF receptor in autophagy initiation. Cell 160(1–2), 145 (2015); University of Wisconsin-Madison press release