Magnetic nanoparticles in cancer therapy: how can thermal approaches help?

The limitations of conventional anticancer therapies (such as moderate therapeutic efficacy, drug resistance, severe adverse reactions, low concentration of therapeutics at the site of action and/or conventional drugs fast renal clearance, etc.) [1] call for novel and often combined anticancer approaches. chemotherapy and radiation therapy are thus increasingly combined with hyperthermia, a local, regional or whole body heating, obtained by microwave, radiofrequency, ultrasound energy or, more recently, magnetism.
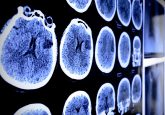
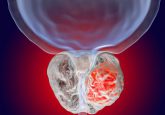
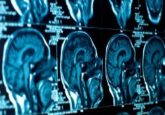
Magnetic hyperthermia relies on the concept that large doses (as sufficient heat could only be obtained by massive nanoparticles administrations) of intratumorally injected magnetic nanoparticles may generate heat after exposure to an external alternating magnetic field and consequently induce cell death within unresectable tumors [2,3]. This method has been used thus far in clinics [4] to treat terminal illness (mainly prostate tumors and glioblastoma multiforme) and the major advantages of this technique are its minimal invasiveness (as the approach requires a single injection of nanoparticles suspension) and its remote application to deep-seated tumors.
Click here to read the full article.